Matters of the Heart: Why Mental Wellbeing Is Cardiac Care
Photo by Eyleen Gomez
February is Heart Month, the Gibraltar Cardiac Association is raising awareness of heart issues and in this article, the last of the month, Jon Santos writes about the link between heart health and mental health.
By Jon Santos
When most people think about heart health, they picture cholesterol numbers, blood pressure cuffs and treadmill stress tests. But cardiologists and psychologists increasingly agree: the state of your mind may be just as important as the state of your arteries.
The relationship between mental wellbeing and the cardiac experience — from prevention to recovery — is not metaphorical. It is biological.
Chronic stress activates the body’s sympathetic nervous system and the hypothalamic–pituitary–adrenal axis, releasing cortisol and adrenaline. In short bursts, this response is adaptive. Over time, however, it contributes to hypertension, inflammation, endothelial dysfunction and increased clotting risk — all central mechanisms in coronary artery disease. Emotional strain literally alters cardiovascular physiology.
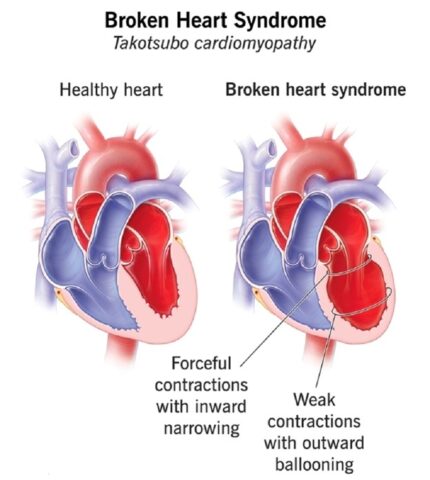
The connection becomes even clearer in conditions such as Takotsubo cardiomyopathy, often called “broken heart syndrome.” Triggered by acute emotional shock — grief, fear or sudden loss — the condition causes temporary weakening of the heart muscle. Imaging shows ballooning of the left ventricle that mimics a heart attack. The cause is not blocked arteries but a surge of stress hormones. It is one of the clearest demonstrations that the heart responds directly to emotional trauma.
Yet the psychological impact of cardiac events may be even more profound than their biological triggers.
After a heart attack, up to one in three patients develops clinically significant depression. Anxiety is common, particularly fear of another attack.
Some individuals experience symptoms consistent with post-traumatic stress disorder: intrusive memories of emergency treatment, sleep disturbance and hypervigilance to bodily sensations. Every skipped heartbeat feels catastrophic. Every chest twinge becomes a threat.
This psychological burden is not simply distressing; it influences life expectancy. Depression following myocardial infarction is associated with higher rates of rehospitalization and mortality. Mechanisms include poorer medication adherence, reduced physical activity and lower heart rate variability — a measure of autonomic flexibility that reflects the body’s capacity to adapt to stress.
Conversely, positive mental health appears to have a protective effect. Individuals with strong social support networks, adaptive coping strategies and a sense of meaning show better recovery trajectories. Cardiac rehabilitation programs increasingly integrate structured exercise with psychological counselling, stress management training and peer support. Participation has been linked to significant reductions in both mortality and depressive symptoms.
Exercise itself offers dual benefits. Aerobic activity improves endothelial function and reduces inflammation while also enhancing mood through neurochemical pathways involving serotonin and endorphins. Mindfulness-based stress reduction has been shown to lower blood pressure and improve emotional regulation. Cognitive behavioural therapy helps patients reframe catastrophic thinking about symptoms and regain confidence in their bodies.
Importantly, mental wellbeing is not only relevant after diagnosis. Preventive cardiology now recognizes chronic workplace stress, social isolation and untreated depression as modifiable risk factors. Screening for psychological distress in primary care and cardiology clinics is becoming standard practice.
The emerging discipline of psychocardiology reflects this shift. It views the heart not as an isolated pump but as part of a dynamic system influenced by emotion, behaviour and social context.
The message is clear: caring for the heart requires caring for the mind. In clinics and communities alike, mental wellbeing is no longer a peripheral concern — it is central to cardiovascular health.









